 As the lethal COVID-19 coronavirus propagates around the globe, we know a sneeze, a cough or simply touching a surface with the virus can spread the infection.
As the lethal COVID-19 coronavirus propagates around the globe, we know a sneeze, a cough or simply touching a surface with the virus can spread the infection.
What researchers don’t know is exactly the role different compositions of mucus, the slimy substance on human tissue, play in the transmission and infection of coronaviruses. Nor do they know why some people known as “super-spreaders” will spread the disease more than others. But University of Utah biomedical engineering assistant professor Jessica R. Kramer is now researching how mucus plays a part in transferring coronaviruses from person to person.
“Not everyone spreads the disease equally. The quality of their mucus may be part of the explanation,” Kramer says. “One person may sneeze and transmit it to another person, and another may not, and that is not well understood.”
She has received a one-year, $200,000 Rapid Response Research (RAPID) grant from the National Science Foundation for the research.
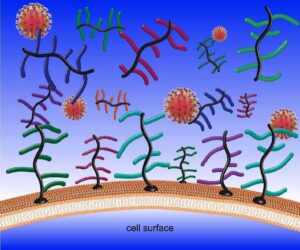 Understanding how different compositions of the proteins that make up mucus spread coronaviruses could help identify those who are “super-spreaders” as well as those who could be more vulnerable to becoming infected, says Kramer. That could lead to faster, more accurate data on who will spread the virus or more effective quarantine measures for high-risk populations. The nation’s epidemiologists have said since the arrival of COVID-19 that accurate testing to know where the infection is growing is a key factor to containing its spread.
Understanding how different compositions of the proteins that make up mucus spread coronaviruses could help identify those who are “super-spreaders” as well as those who could be more vulnerable to becoming infected, says Kramer. That could lead to faster, more accurate data on who will spread the virus or more effective quarantine measures for high-risk populations. The nation’s epidemiologists have said since the arrival of COVID-19 that accurate testing to know where the infection is growing is a key factor to containing its spread.
Kramer and her team will create different forms of synthetic mucins, the proteins that make up mucus, and test them with non-hazardous versions of coronaviruses. COVID-19, which is the cause of the worldwide pandemic, is a novel coronavirus that by the end of March has so far killed more than 37,000 people since it was first discovered late last year. But it is only one of many forms of coronaviruses.
Kramer will use special aerosols in a closed environment to simulate coughing to help determine how different mucins carry the virus through the air. She will also test the viability of the virus when it lands on a surface based on the mucins that carry it. Her lab will also examine how mucin composition on the next victim’s mouth, eyes or lungs affects whether the virus makes it through the mucus into their cells to replicate.
The composition of mucus changes from person to person based on their genetics, environmental factors, or their lifestyle such as whether the person smokes or what their diet is.
“It’s important that people understand that it’s not only the amount of mucus that is a factor but how the molecular composition is different,” she says.
Kramer’s lab at the University of Utah has been creating synthetic mucins and more recently studying how mucins and bacteria interact with each other. She says researching how mucins interact with viruses is a natural extension of this work.
Kramer’s award is the second NSF RAPID grant to be given to U researchers related to the spread of the COVID-19 coronavirus. Michael Vershinin and Saveez Saffarian of the U’s Department of Physics & Astronomy will study how the structure of the coronavirus withstands changes in humidity and temperature and under what conditions the virus falls apart.